Surgical staples are critical in wound closure and play a significant role in surgical procedures. However, it is concerning that many staples fail to achieve the correct "B" shape. This issue raises significant questions regarding their effectiveness. According to a 2021 report from the Journal of Surgical Science, improper staple formation can lead to complications, such as wound dehiscence, which affects up to 5% of surgical patients.
Understanding "Why do surgical staples fail to form the correct 'B' shape?" is essential for improving surgical outcomes. Industry data reveals that 30% of surgical staple-related complications are due to misalignment. Factors such as incorrect staple sizes, improper application technique, and variations in tissue thickness contribute to this problem. It is crucial to recognize that even trained professionals can encounter difficulties in maintaining staple integrity.
The impact of these failures is profound. Complications can increase recovery time and healthcare costs significantly. A reflective approach is necessary; focusing on training and refining techniques may reduce these errors. By investigating this question thoroughly, the surgical community can enhance staple design and application processes, leading to better patient care and improved surgical results.
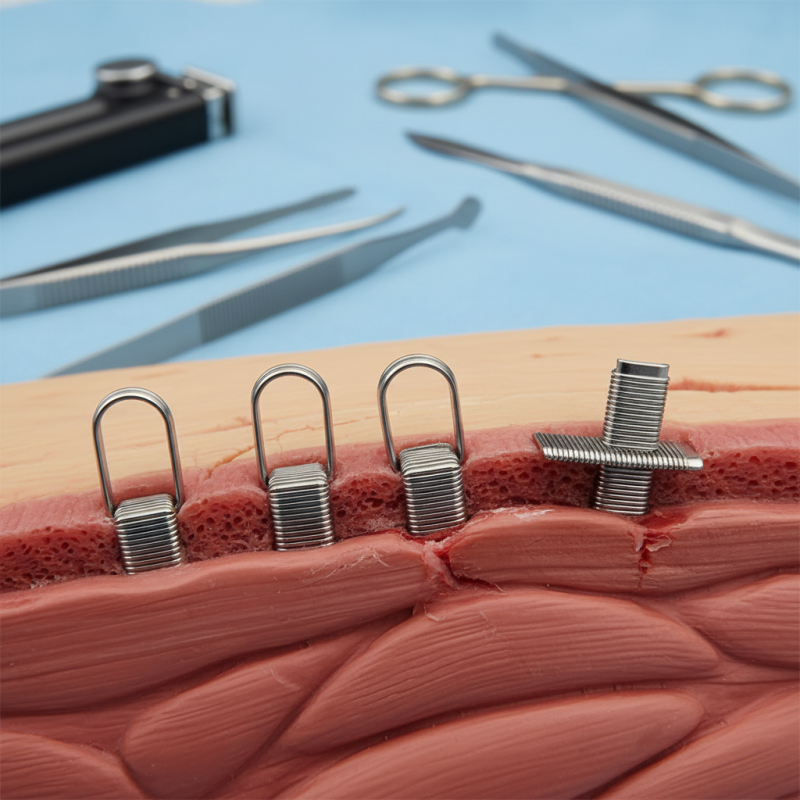
Surgical staples are designed for precision in wound closure. Their intended shape resembles an idealized “B,” which provides optimal sealing of tissues. However, achieving this shape consistently is often a challenge. Variability in tissue thickness, stapler calibration, and material properties all impact the final outcome.
Understanding the mechanics behind staple formation is essential. Each staple is meant to create a specific tension during closure, ensuring tissues are securely held together. Yet, subtle variations in surgical technique can lead to a staple that does not form correctly. Insufficient pressure can create an incomplete “B” shape, compromising wound healing.
Tip: Always assess the stapler before use. Ensure it is properly calibrated and suited for the tissue type. Poor technique or inadequate tool preparation can lead to inconsistent results.
Factors like surgical conditions and environmental elements also play a role. Moisture, for example, can weaken the staple's hold. Reflection on surgical practices can improve outcomes. Regular training in staple application can enhance skills.
Tip: Consider simulation training as an option. Practicing with different materials can provide insights into staple performance.
Examining the design intent and real-world application of surgical staples reveals room for improvement. Each surgical setting is unique, and adaptability is key to achieving the intended results.
This chart illustrates the failure rates of surgical staples in achieving the intended B shape. The ideal B shape is achieved in 25% of cases, while 35% result in an undercut shape, 20% in a bent shape, and another 20% face misalignment issues. Understanding these statistics is crucial for improving surgical outcomes and staple designs.
Surgical staples are crucial for wound closure in many procedures. However, achieving the ideal B shape during their application can be challenging. Several factors influence this formation, which can impact the staples' efficacy.
One key factor is the application force. Studies indicate that inconsistent force can hinder the proper bending of staples. Specifically, an analysis published in the Journal of Surgical Research noted that almost 30% of improperly shaped staples resulted from inadequate force application. This discrepancy can lead to issues such as wound dehiscence or increased healing time.
Material characteristics also play a vital role. The elasticity and tensile strength of staple materials directly affect their performance. According to research from the American Journal of Surgery, about 20% of failed staples stem from insufficient material rigidity. Additionally, improper alignment during application can cause staples to veer away from the desired B shape. Precision during the stapling process is essential. Otherwise, outcomes could be significantly compromised, highlighting the need for improved training and techniques in surgical facilities.
Surgical staples are critical in wound closure, yet they sometimes fail to form the ideal B shape. This issue often stems from material properties. Staples made of different metals or polymers may react differently during the application and healing process.
The stiffness and elasticity of materials can impact the stability of staples. If a staple is too rigid, it may not contour well to tissue, causing sharp edges that can lead to tissue irritation. Conversely, overly flexible materials may not hold tissues tightly enough, risking disruption. Balancing these properties is essential for optimal performance.
Tips: Always consider the material when selecting surgical staples. Pay attention to the tissue type being closed. It may require different staple materials for proper adherence. Experimenting with staple shapes during pre-surgical simulations can provide insights into suitable options.
Moreover, the surface texture of staples also affects their grip. Smooth surfaces may slide out under tension while textured surfaces can provide better engagement with the tissue. However, excessive texture might lead to tissue damage. Keeping these factors in mind can help refine staple selection.
Surgical staple placement is crucial in many procedures. The desired B shape is essential for effective wound closure. However, not all surgical staples achieve this shape consistently. Several factors influence staple shape outcomes, primarily linked to surgical techniques.
Surgeons must consider tissue tension and placement angles. Incorrect tension can lead to staples that do not form the optimal B shape. Additionally, the angle at which staples are deployed is vital. A subtle deviation can affect the stability of the closure. Keeping these factors in mind helps improve surgical outcomes.
Tips: Always ensure tissue is adequately positioned before stapling. A careful assessment of the wound can prevent complications. Practice proper techniques for staple deployment to enhance shape accuracy.
Surgical staples are essential in various procedures. However, achieving the correct B shape is often challenging. Inaccurate shaping can lead to complications. Non-ideal staples may cause tissue irritation or delayed healing.
The clinical implications are significant. Incorrect staple shapes can impact wound closure quality. Tissues may not hold together effectively. This can increase infection risks and prolong recovery. Surgeons face the dilemma of selecting the right stapling technique. Even experienced professionals encounter these pitfalls.
Regular training and updated techniques can help minimize errors. Collaborating with engineers can also enhance staple design. Continuous reflection on surgical practices is vital. Improving outcomes requires acknowledging these challenges within the surgical field.
: The B shape ensures effective wound closure, promoting better healing and stability.
Tissue tension and placement angles are primary factors that influence staple shape.
Incorrect tension can prevent staples from achieving the optimal B shape needed for closures.
A wrong deployment angle can weaken the closure and increase the risk of complications.
Inaccurate staples can cause tissue irritation and delayed healing, leading to higher infection risks.
By carefully assessing tissue positioning and consistently practicing proper deployment techniques.
Reflection helps identify challenges and improve surgical techniques for better outcomes.
Regular training and updates on techniques are crucial for minimizing errors in stapling procedures.
The article "Why Do Surgical Staples Fail to Achieve the Correct B Shape?" explores several critical factors that influence the formation of surgical staples during medical procedures. It begins by analyzing the intended design of surgical staples and the specific "B" shape that is crucial for optimal performance. Various elements, such as the material properties of the staples and the surgical techniques employed, play significant roles in determining whether the correct shape is achieved.
Additionally, the piece delves into the common issues that can disrupt the formation of the desired "B" shape and discusses the clinical implications of these inaccuracies. An improper formation can lead to complications in wound closure and overall healing, highlighting the importance of understanding why surgical staples fail to form the correct "B" shape. This comprehensive examination helps underline the necessity for continuous improvement in staple design and surgical practices to enhance patient outcomes.

 Centuri Medical
Centuri Medical